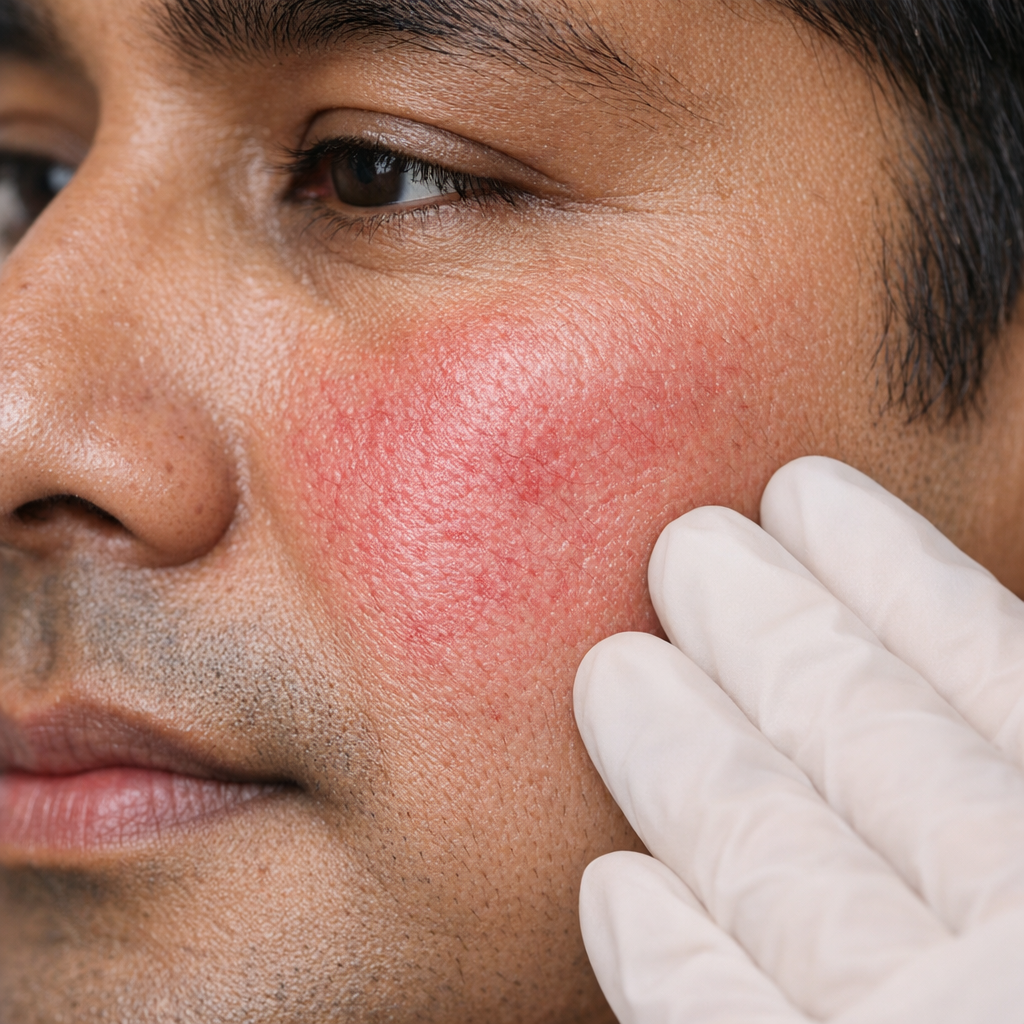
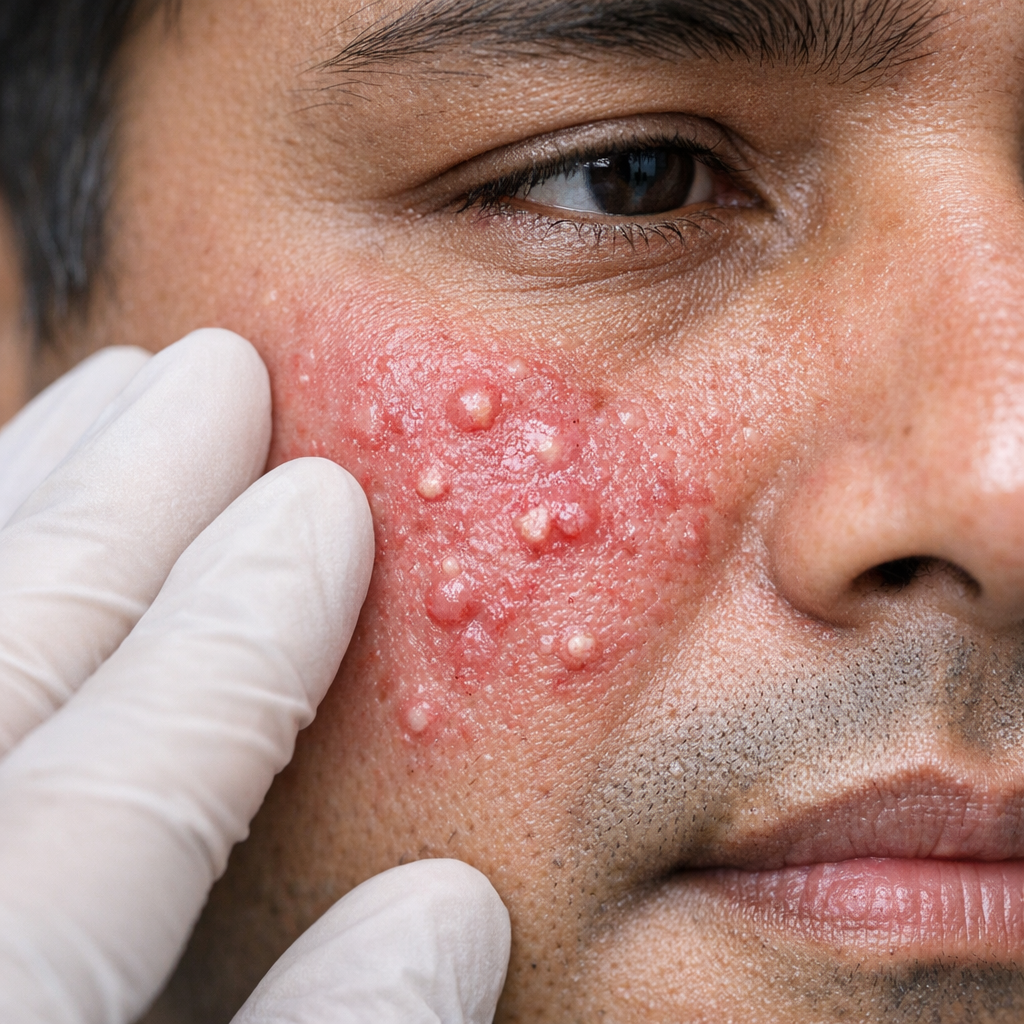
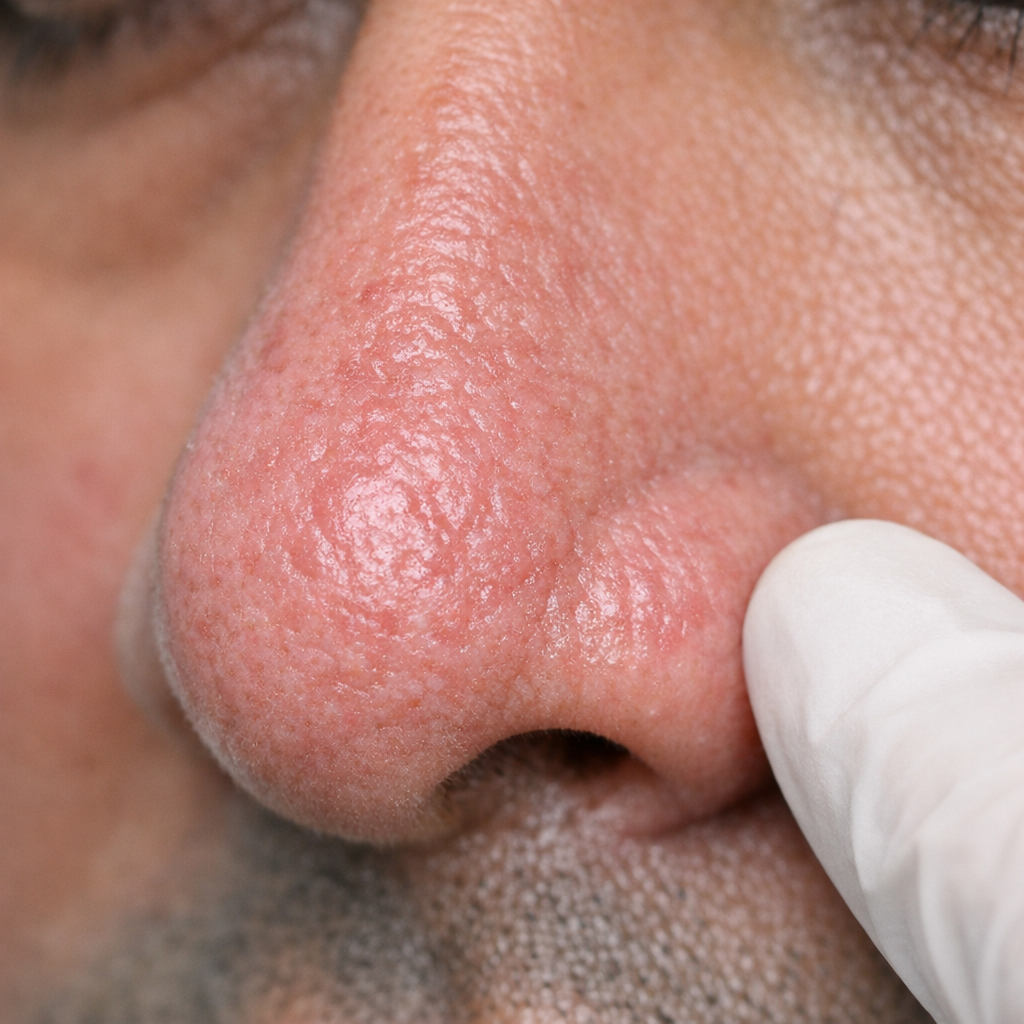
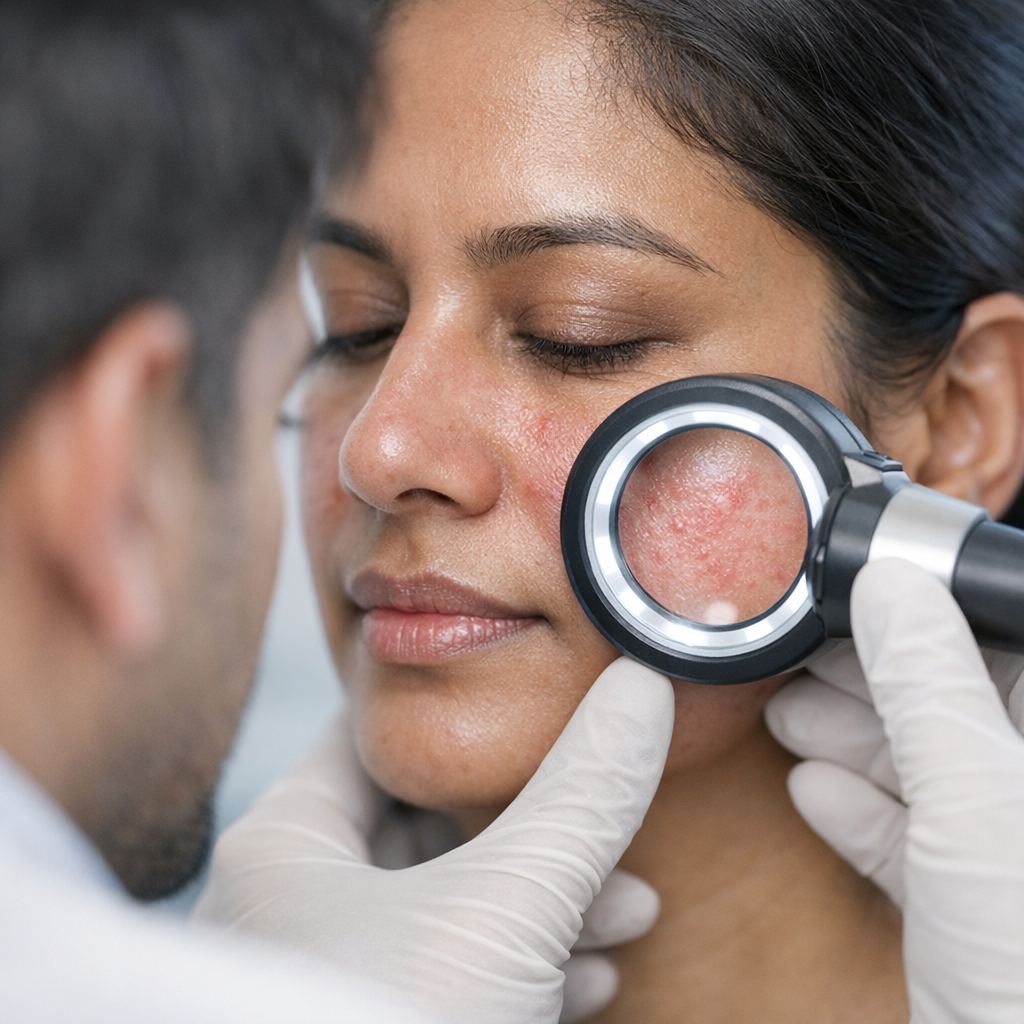
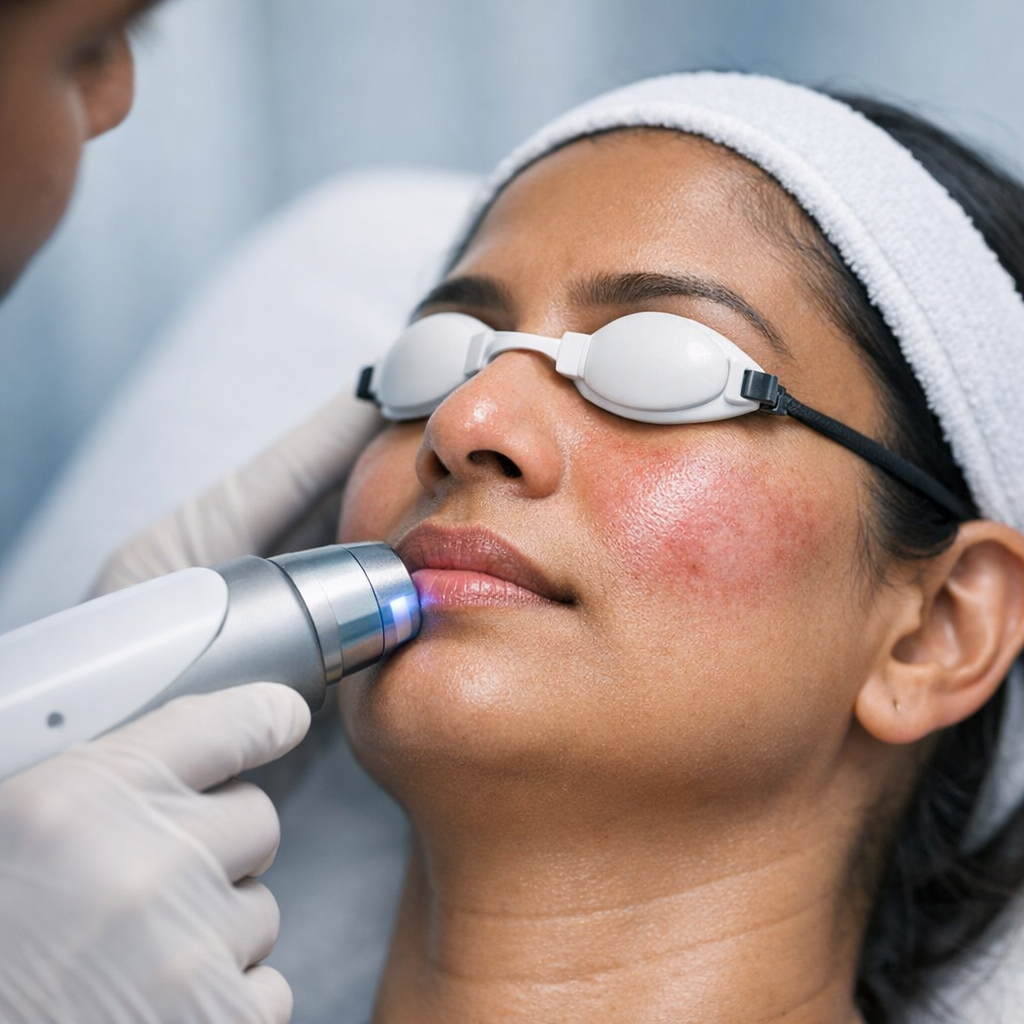
Rosacea &
Sensitive Skin
Persistent facial redness, visible blood vessels, pustules that look like acne but won't respond to acne treatment — rosacea is chronic but very controllable with the right triggers identified and the right topicals prescribed.