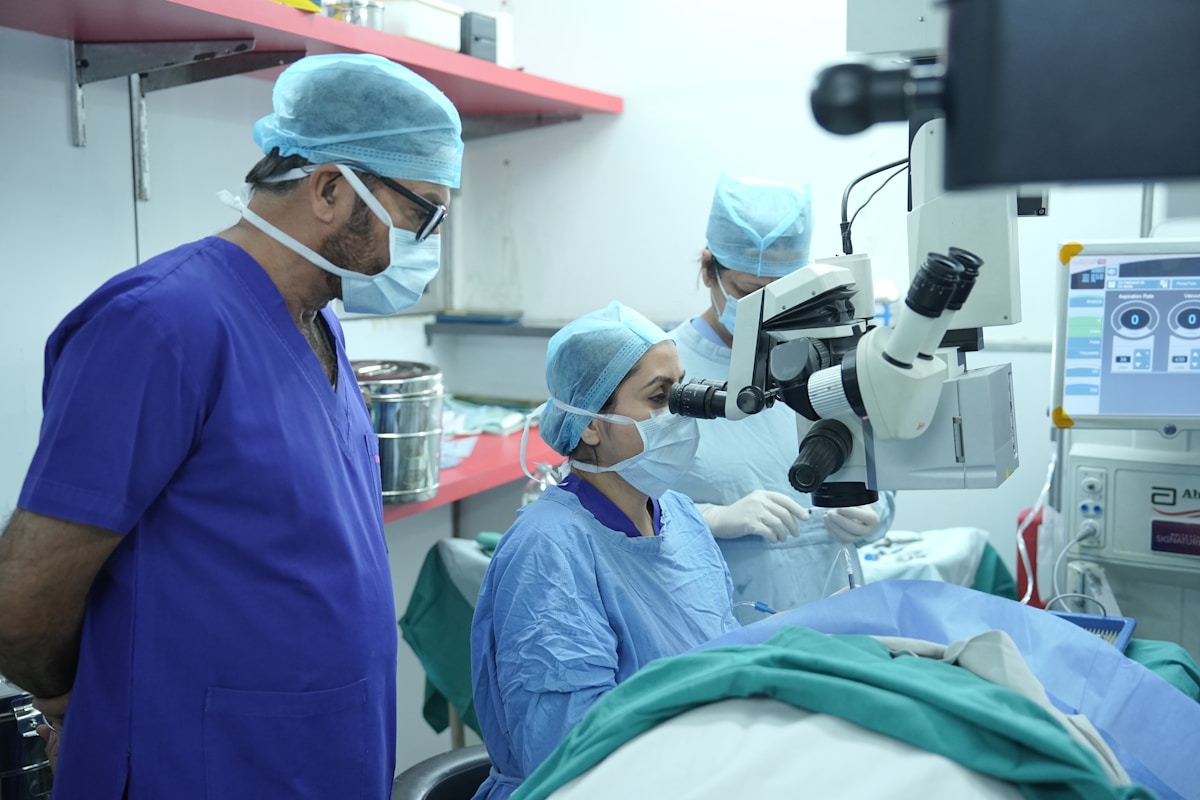
Retinal
Care
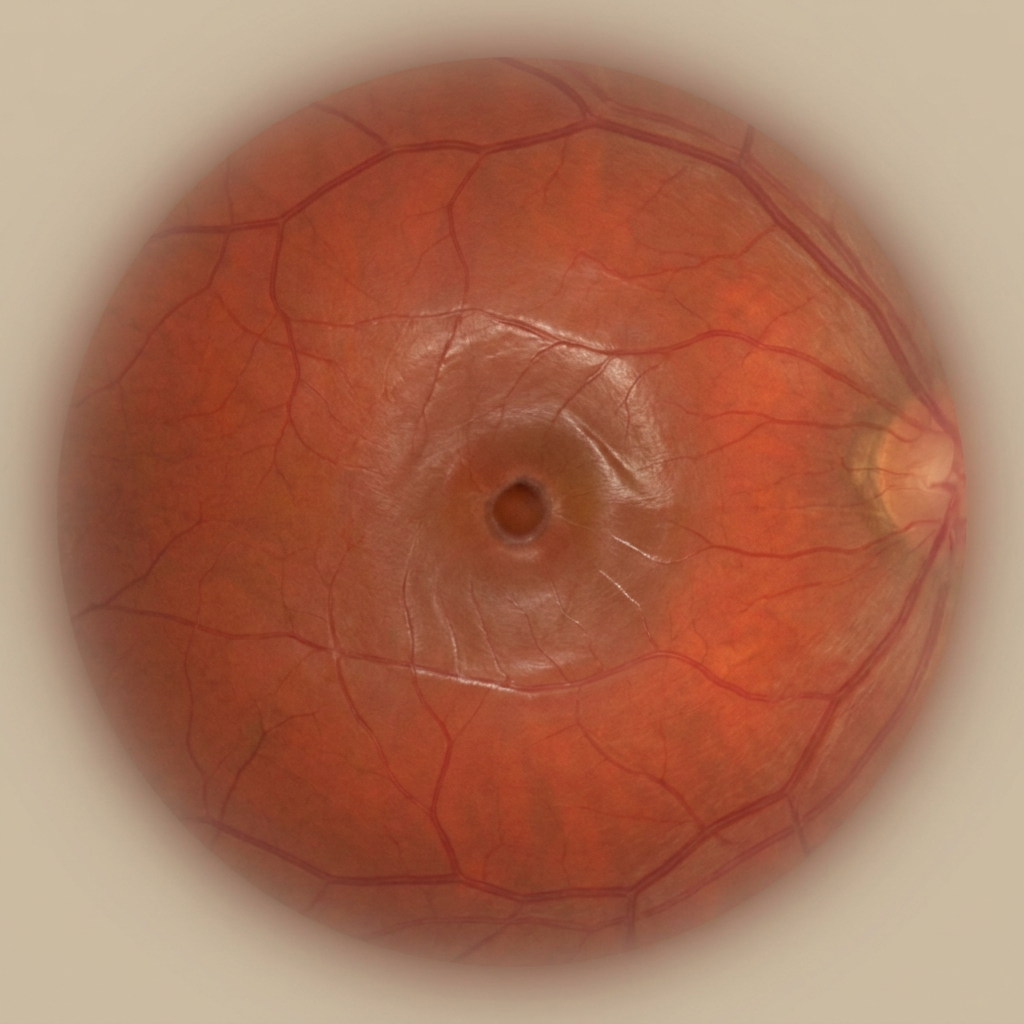
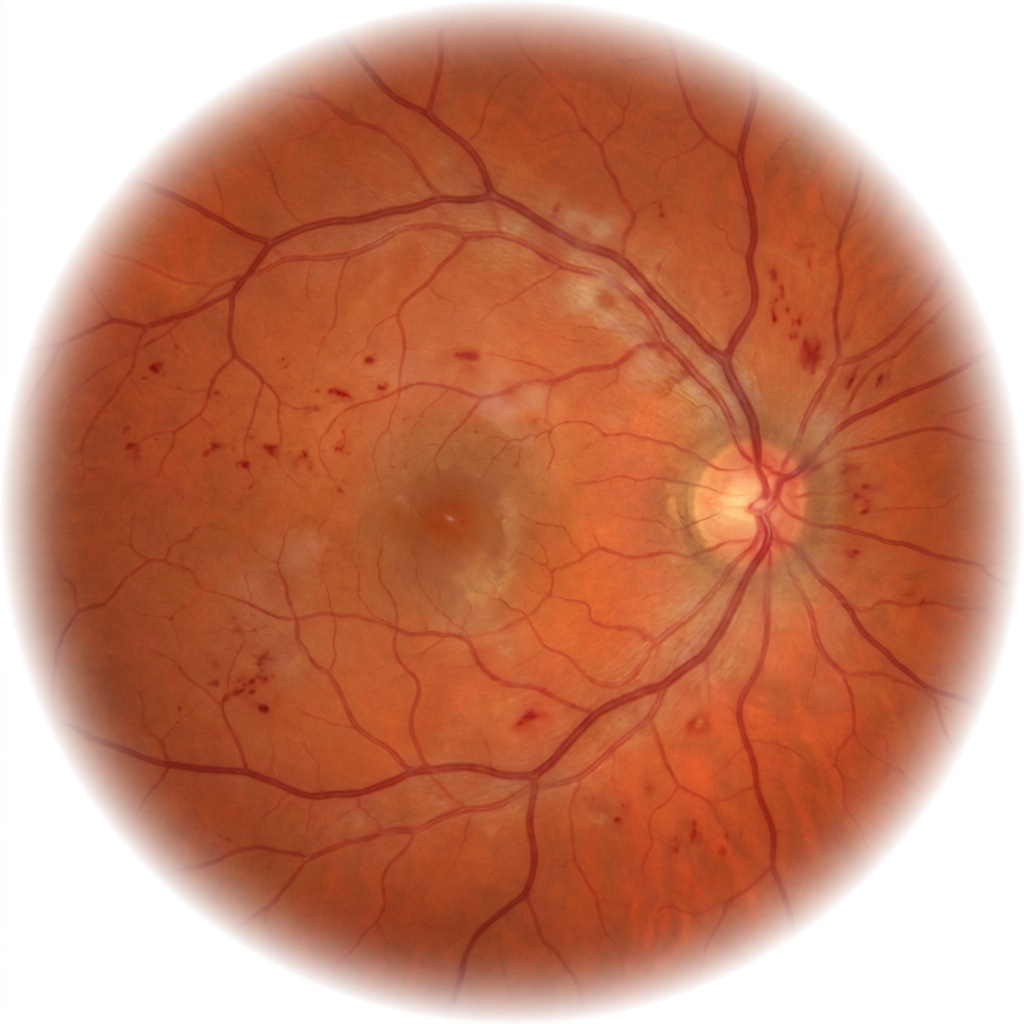
The retina is the camera film of the eye — once it is damaged, vision lost cannot be recovered. Anti-VEGF injections, retinal laser, and vitreoretinal surgery can halt progression and, in many cases, restore significant sight.