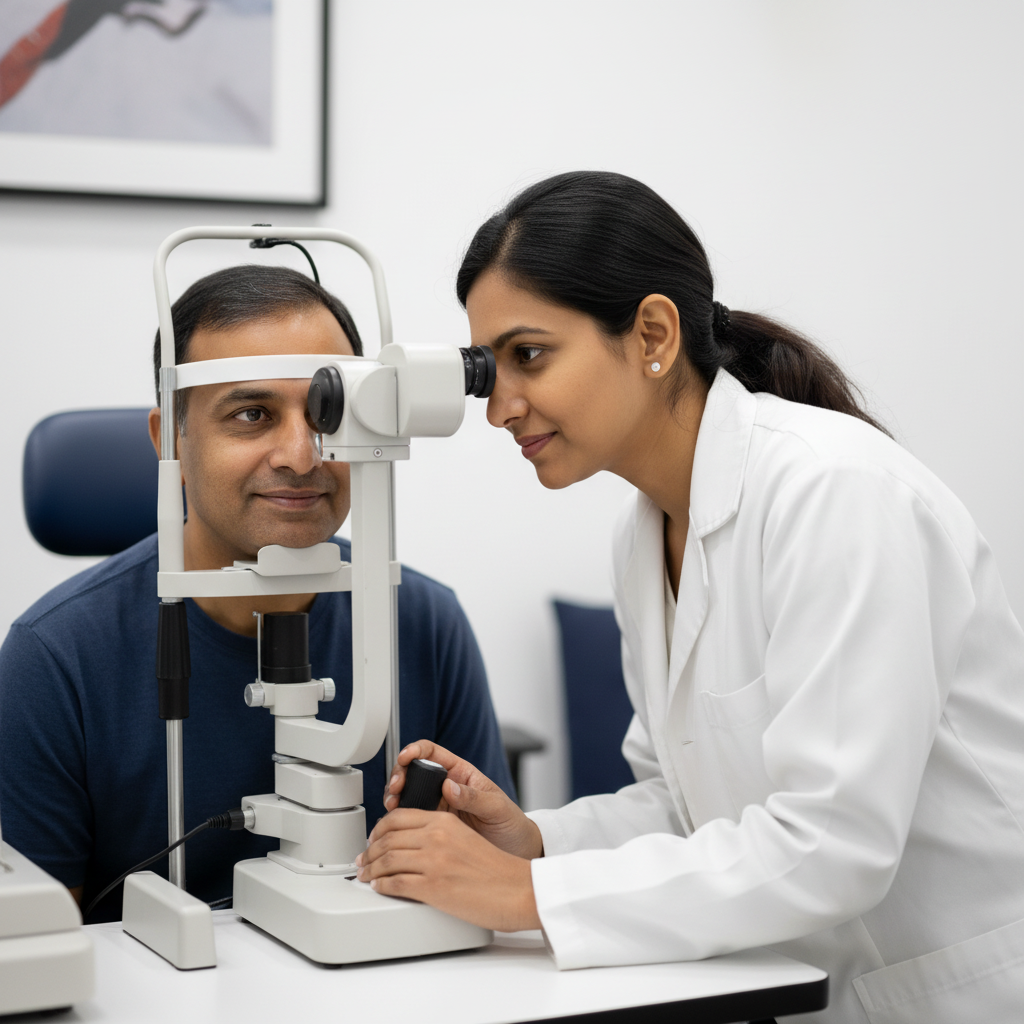
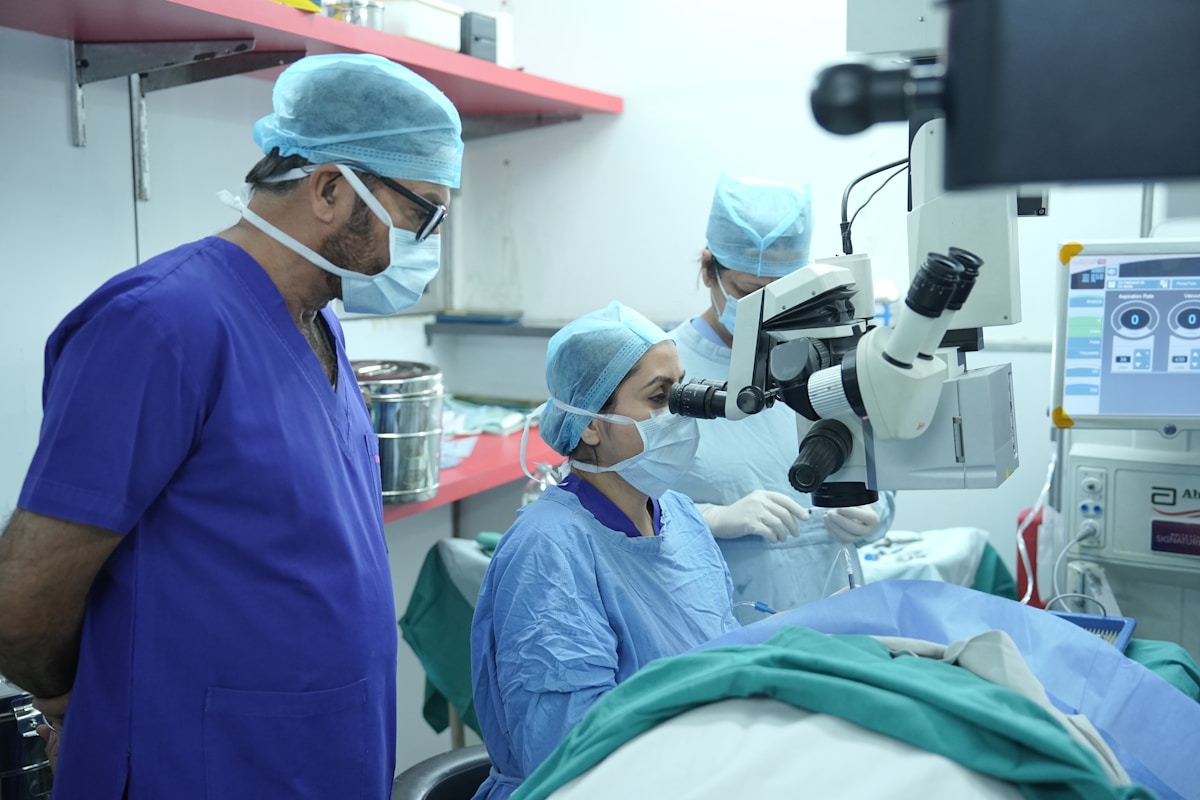
Diabetic Eye
Screening
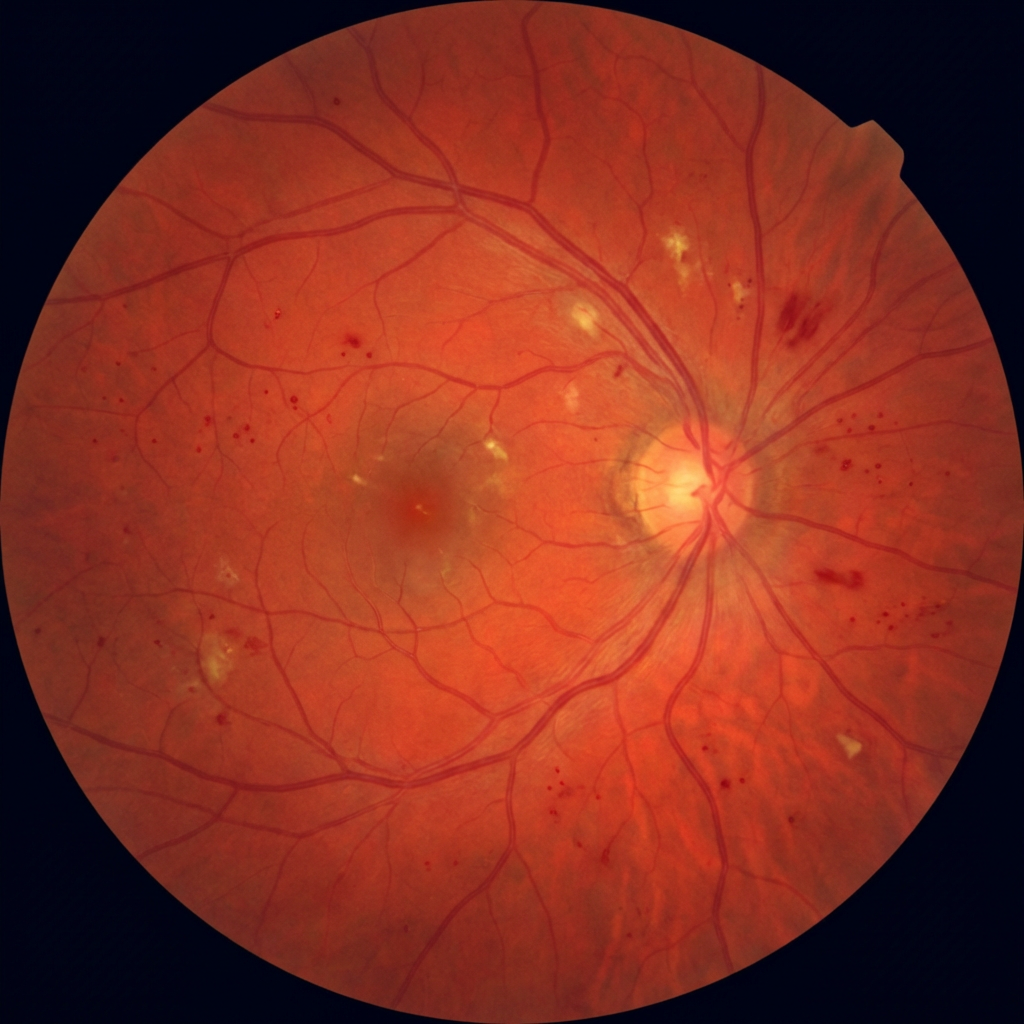
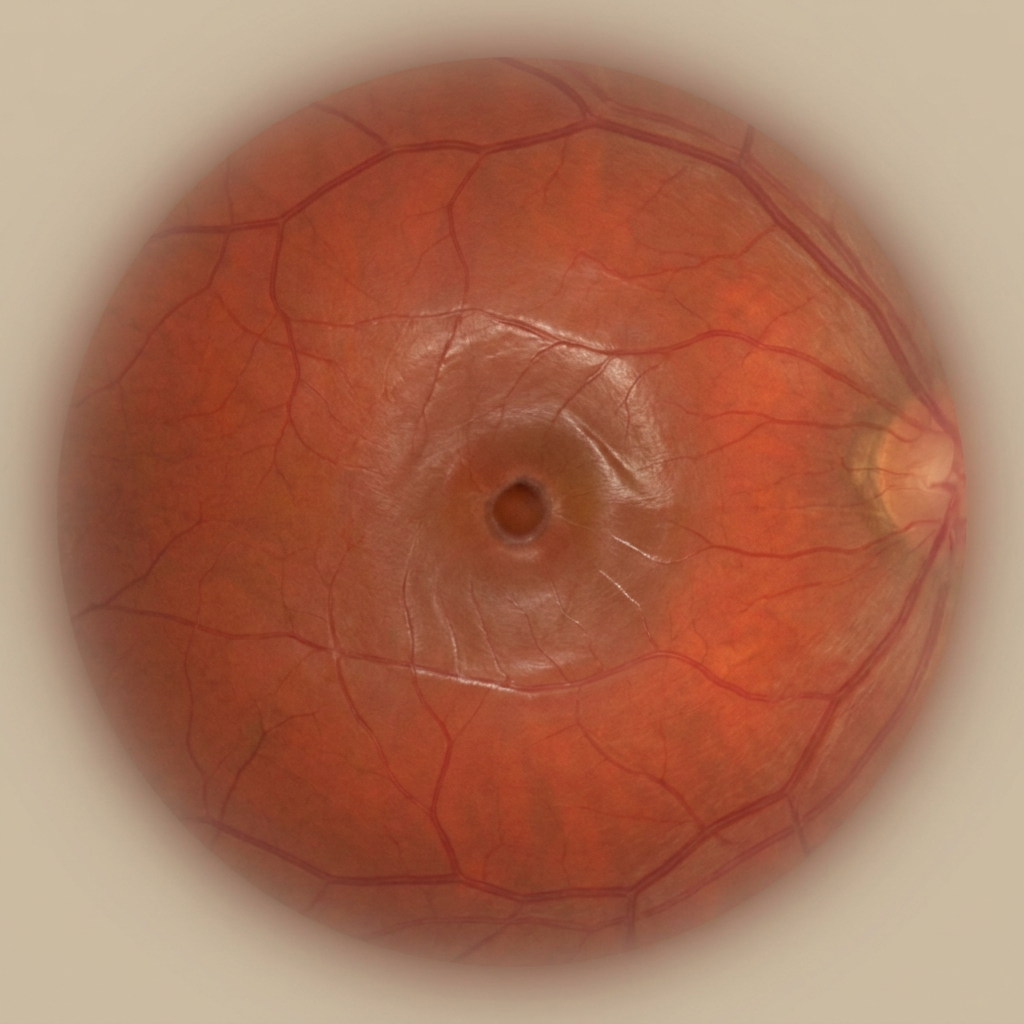
90% of diabetic blindness is preventable with annual screening and timely treatment. Diabetic retinopathy causes no symptoms until it is advanced — by the time your vision blurs, significant and often irreversible damage has already occurred.