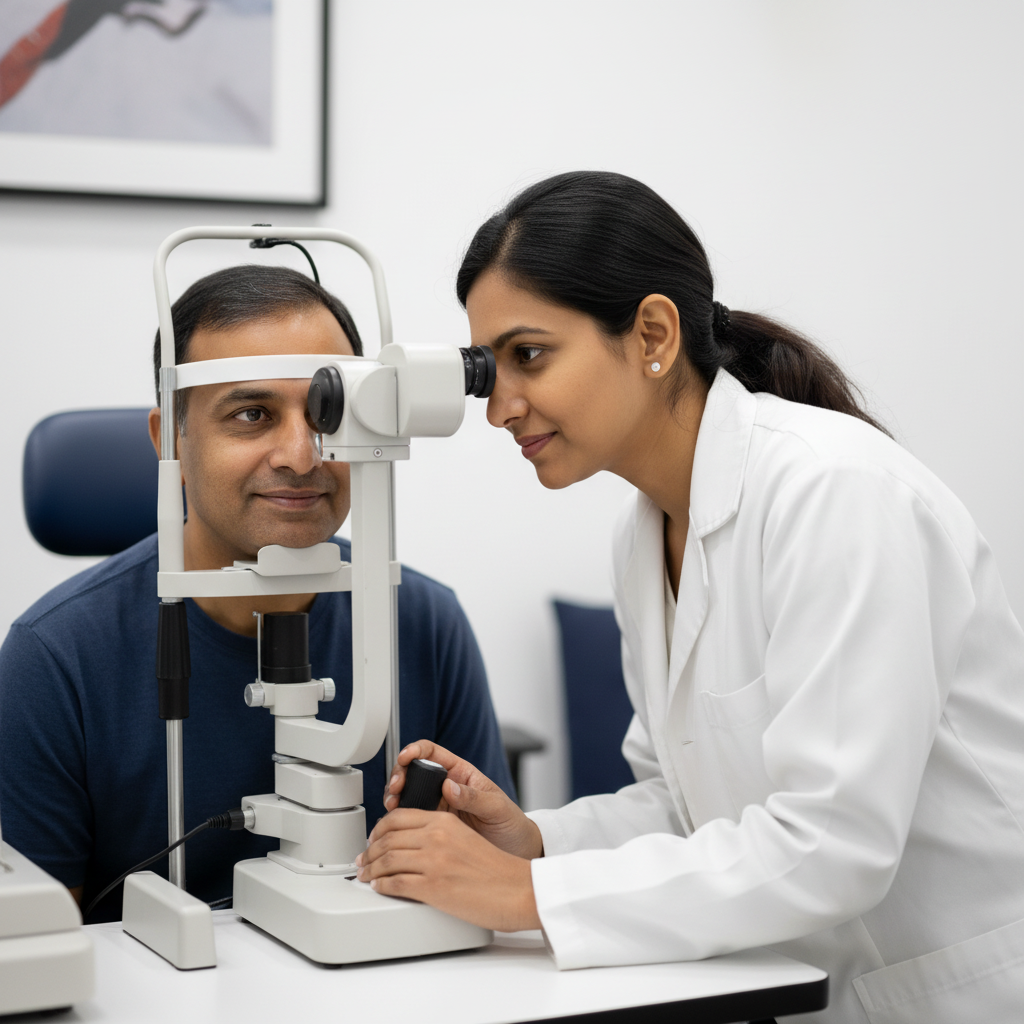
Dry Eye
Treatment
Dry eyes are not just discomfort — chronic inflammation damages the ocular surface and can reduce visual quality significantly. 85% of cases stem from Meibomian gland dysfunction, not reduced tear production. Treatment must target the root cause.