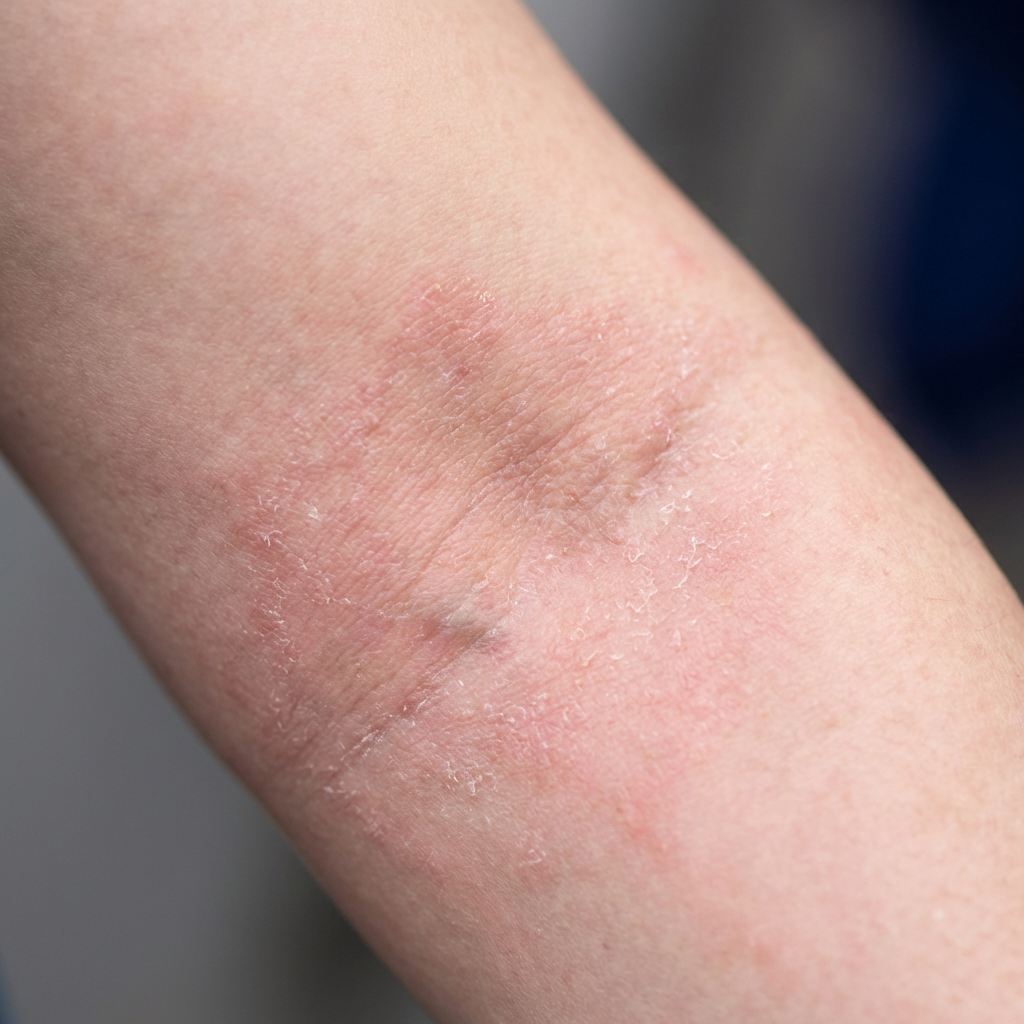
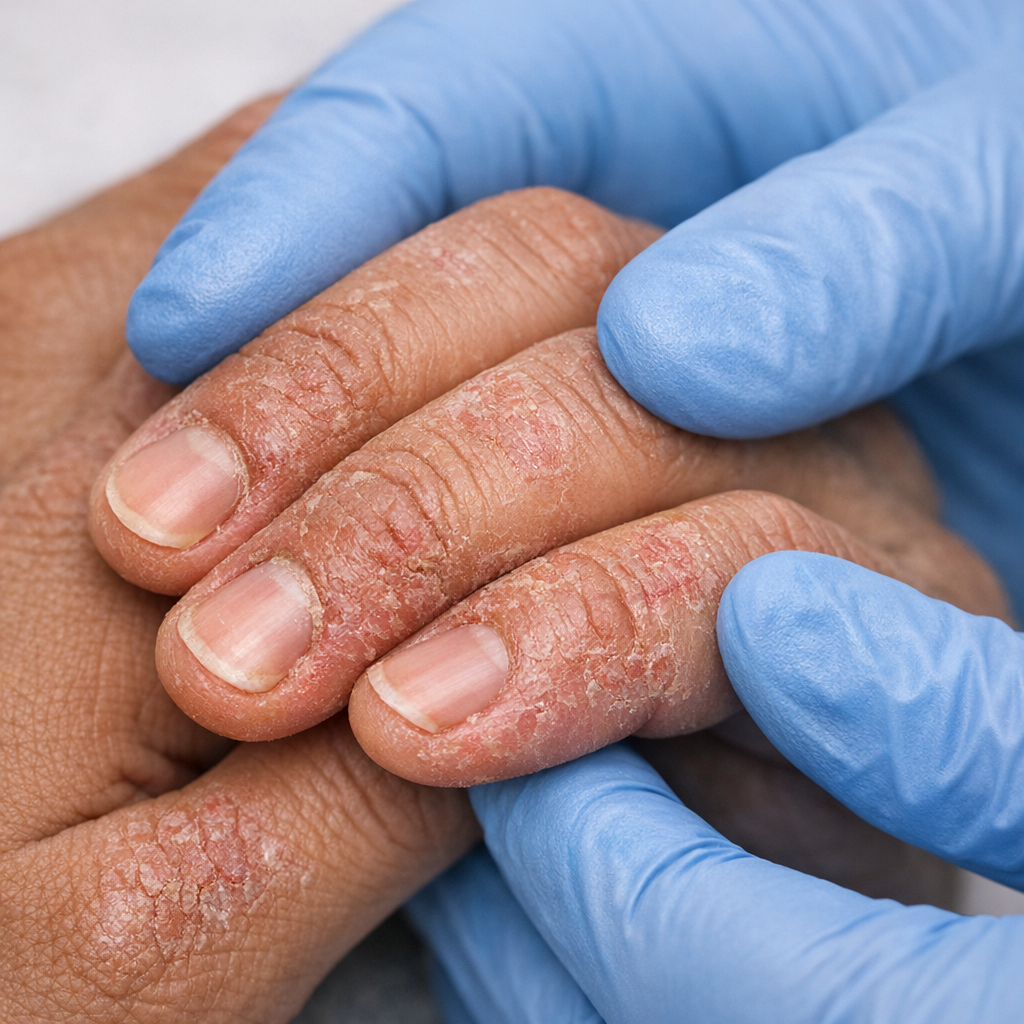
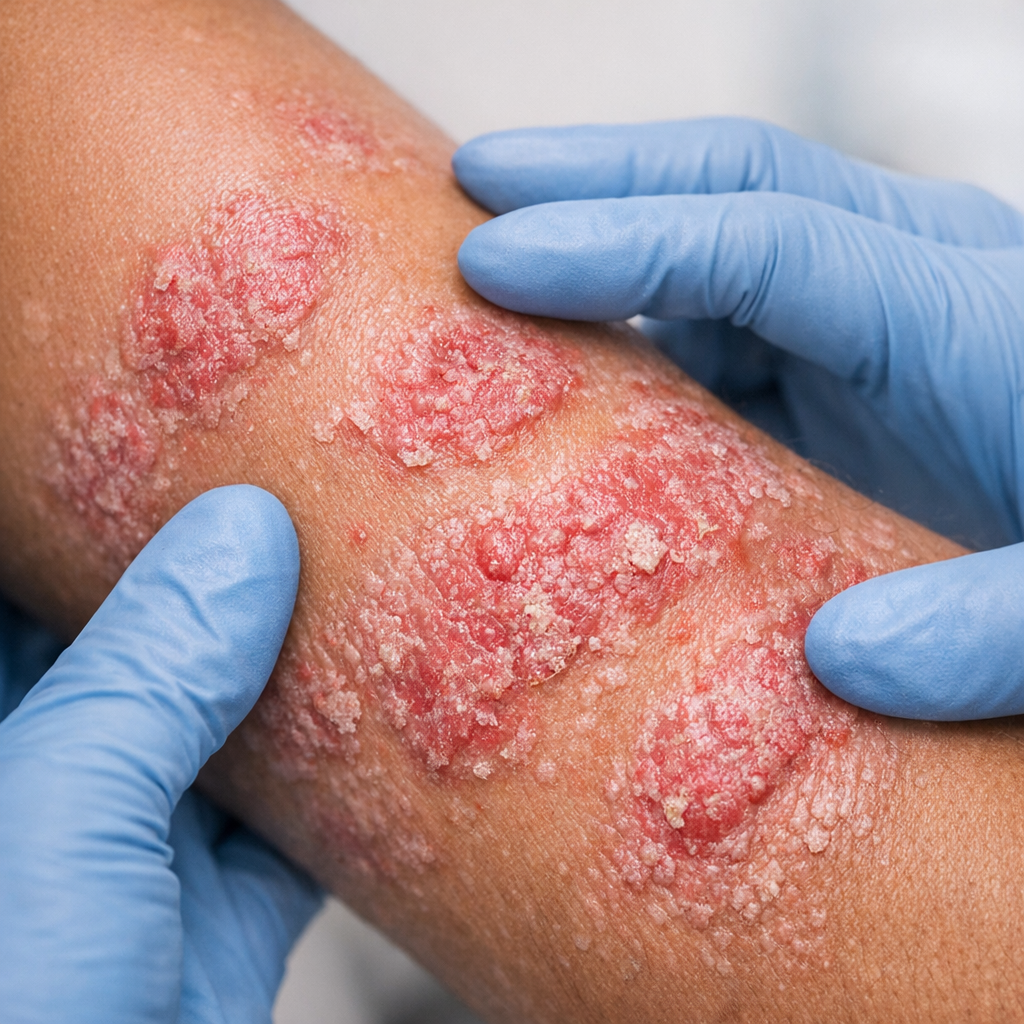
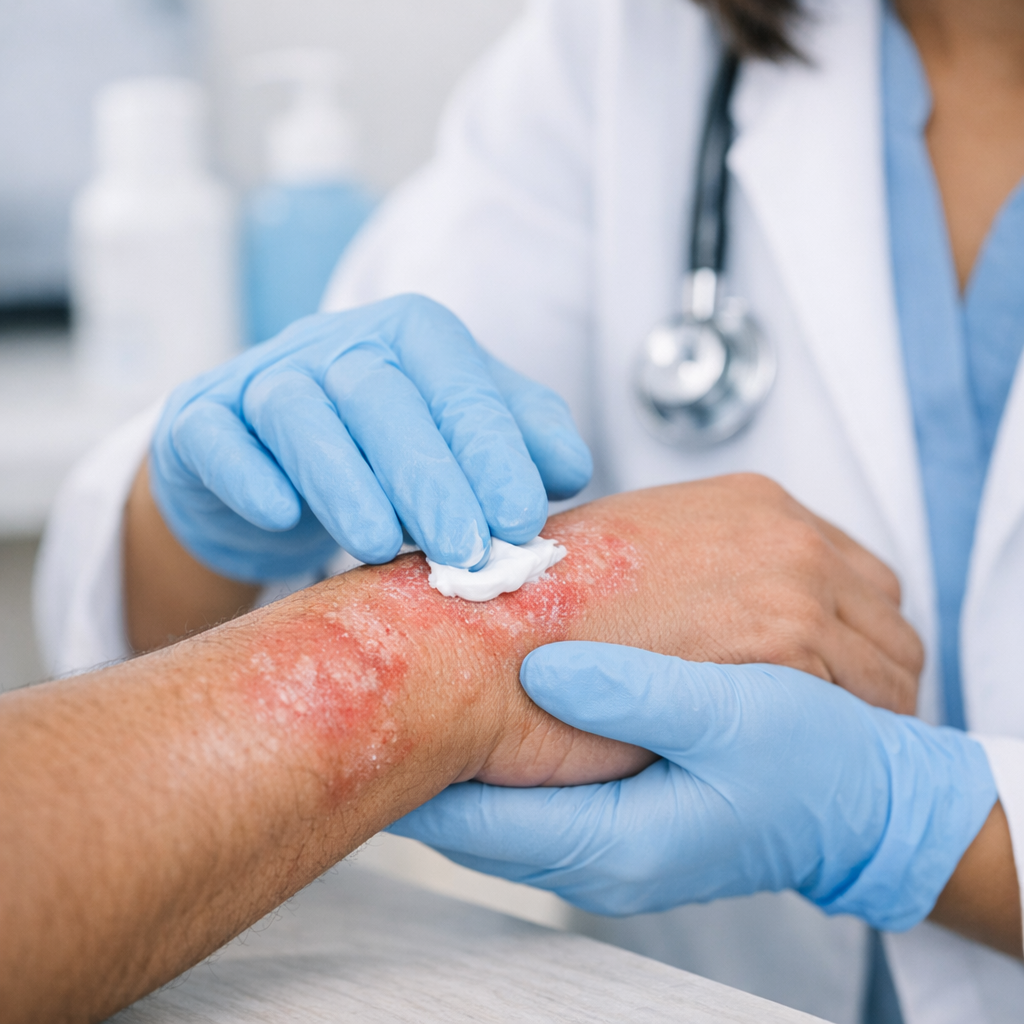
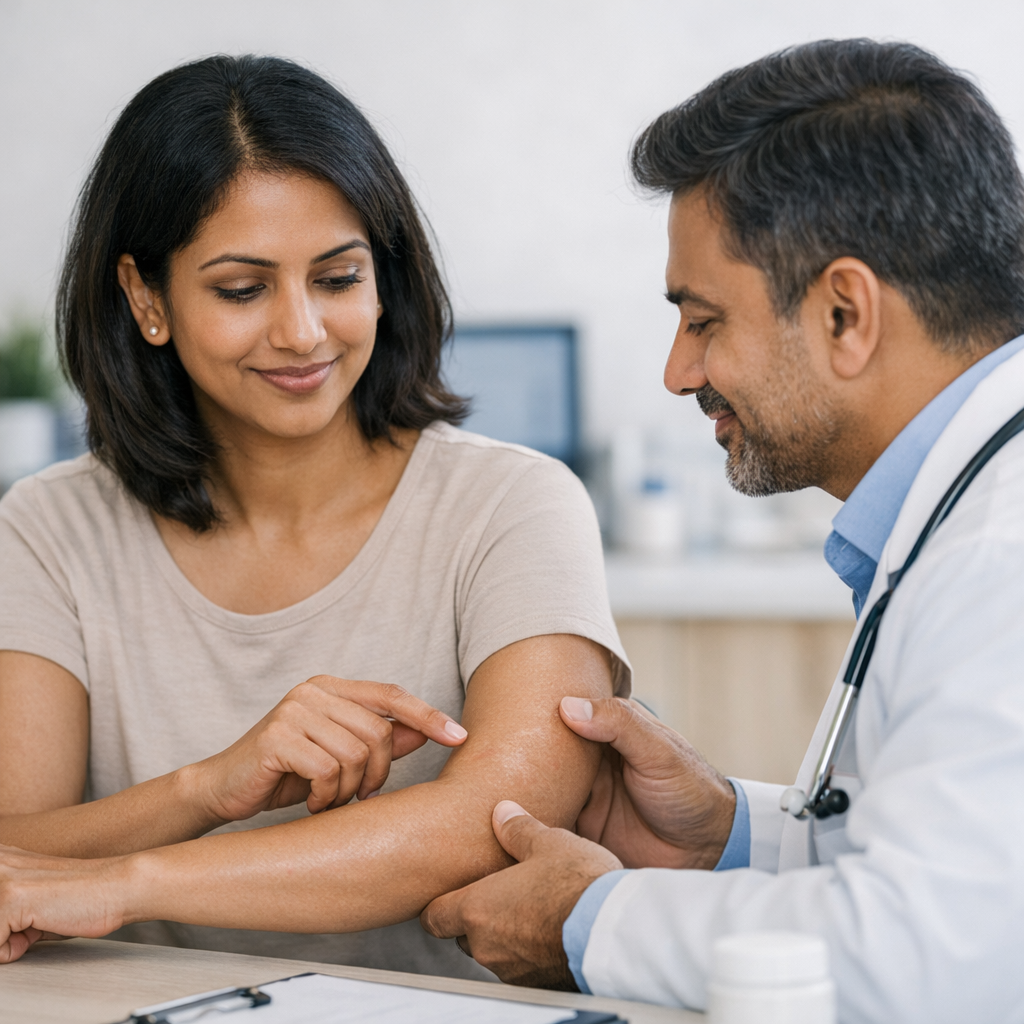
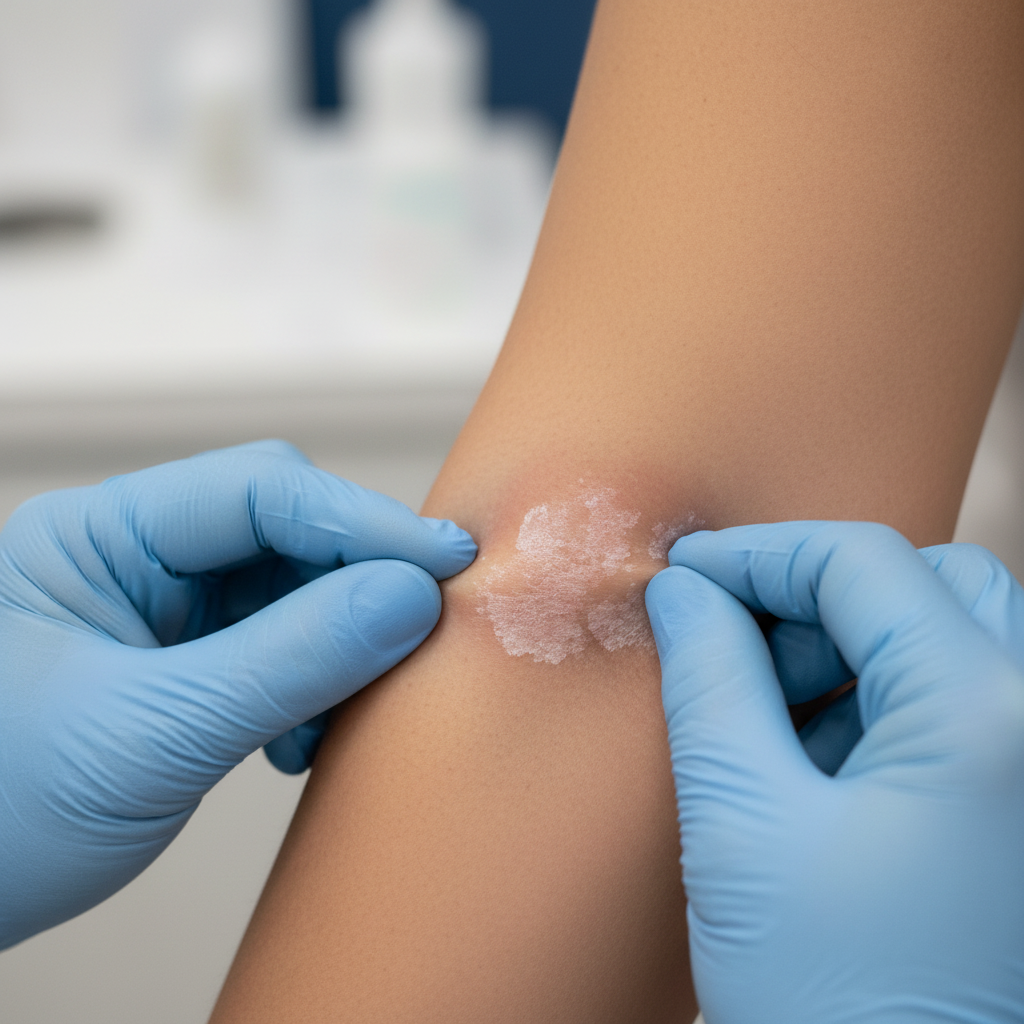
Eczema &
Atopic Dermatitis
Persistent itch, inflamed skin, and recurring flares don't have to be your reality. We identify your specific triggers, prescribe the right barrier repair and immunomodulator therapy, and build a personalised flare-prevention plan.